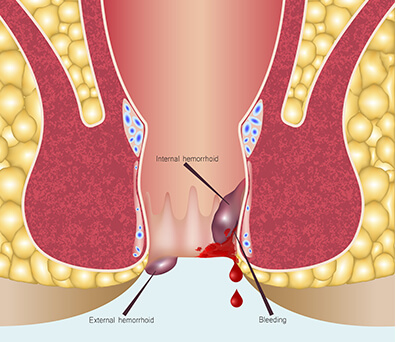
An anal fissure is a small tear near the lining of the anal canal. It can cause severe pain and bleeding after the bowel movements. The bleeding can vary from light to heavy bleeding. Anal fissures are often mistaken for hemorrhoids because they both have similar symptoms. Anal fissures are a common problem, and they can occur in infants, young children, and adults. Based on research, anal fissures occur in women from 12 to 24 years of age – in men, they can occur from 55 to 64 years of age. Anal fissures can last for more than six weeks (acute anal fissure) – but if persistent, anal fissures can become a chronic condition. Anal fissure causes discomfort and pain, but there are treatment options that can relieve these symptoms.
Causes of Anal Fissure
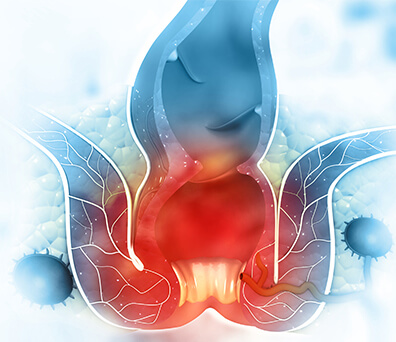
An injury to the lining of the anal canal or a hard bowel movement (commonly in cases of constipation) usually causes anal fissures. It occurs because of a trauma to the inner lining of the anus, which causes stretching of the anal canal. Also, in some cases, no clear cause is identified. Other possible causes are listed below.
-
 Constipation (large, hard stool can cause lesions in the anal area).
Constipation (large, hard stool can cause lesions in the anal area). -
 Persistent diarrhea.
Persistent diarrhea.  Inflammatory bowel disease (such as Crohn’s disease and ulcerative colitis).
Inflammatory bowel disease (such as Crohn’s disease and ulcerative colitis).  Having an unusually tight anal sphincter muscle (increased tension in the anal canal makes it more susceptible to tearing).
Having an unusually tight anal sphincter muscle (increased tension in the anal canal makes it more susceptible to tearing).  Pregnancy and childbirth.
Pregnancy and childbirth.  Sexually transmitted infections (STI) can cause infection and damage the anal canal.
Sexually transmitted infections (STI) can cause infection and damage the anal canal.
Anal fissures do not heal easily because the pain felt during a bowel movement can cause a spasm of the sphincter muscle and decrease the blood flow to the area, which interferes with the healing process. This cycle is repeated with each bowel movement, resulting in more pain, more spasms, and even less blood flow each time you pass stool.
Some other causes of an anal fissure are listed below:
-
 Straining during bowel movements.
Straining during bowel movements. -
 Prior anal surgery.
Prior anal surgery.  Anal intercourse.
Anal intercourse.  Tumors.
Tumors.
Symptoms of Anal Fissure
The most common symptom of an anal fissure is an intense and sharp pain in the anal during defecation, which is followed by a deep, burning sensation that can last for several hours. Most people notice bright red blood (fresh blood) in or on the surface of their stools or the toilet paper.
The symptoms of Anal Fissure are as follows:
-
 A sharp pain during feces .
A sharp pain during feces . -
 A deep burning pain that can last for several hours,
A deep burning pain that can last for several hours,  Mild or heavy bleeding may occur in feces or on the toilet paper.
Mild or heavy bleeding may occur in feces or on the toilet paper.  Pain during a bowel movement.
Pain during a bowel movement.
Treatment of Anal Fissure
Anal fissures typically can heal within a few weeks without medical intervention. However, they can quickly reoccur if the underlying cause is not treated. In some cases, medicines such as pills, suppositories, creams, or gels may be prescribed to help relax the sphincter muscles and accelerate the healing process. Topical anesthetics may help ease the pain and relax the sphincter, as well as soaking in sitz baths after a bowel movement. Surgery may be recommended for persistent cases of anal fissures where home remedies and medical treatment have not been successful.
Prevention of Anal Fissures
Preventing and treating anal fissures begins with changes in diet to help form a softer stool that is easier to pass. A high fiber diet makes stool bulkier while drinking more water, and taking a stool softener can help stool pass more easily; this will reduce straining and allow the fissure to heal. The fear of pain may cause people to postpone having a bowel movement, but this can cause the stool to become harder, increasing the risk of constipation and tears. Going to the washroom when you feel the urge to will aid in preventing anal fissures and also promote healing in existing fissures. Frequent or regular exercise can also aid in preventing constipation. It is also recommended to avoid straining and sitting on the toilet for an extended period.
References:
-
 https://www.mayoclinic.org/diseases-conditions/anal-fissure/symptomscauses/syc-20351424
https://www.mayoclinic.org/diseases-conditions/anal-fissure/symptomscauses/syc-20351424 -
 https://www.nhs.uk/conditions/anal-fissure/
https://www.nhs.uk/conditions/anal-fissure/
Speak to a Canadian pharmacist about your symptoms

CALL(TOLL-FREE)

